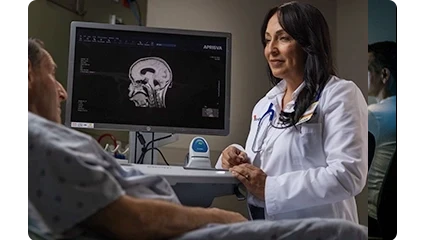
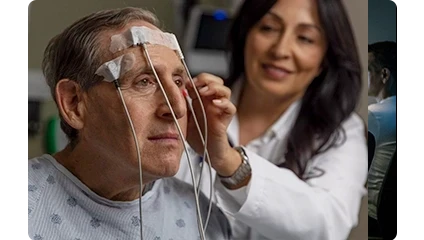
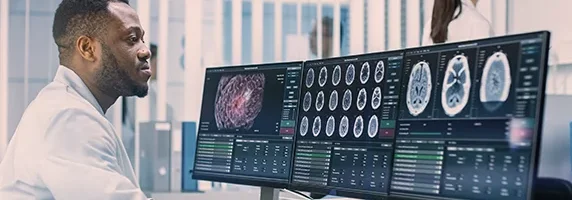
Augment neurological care to meet community need
Whether you’re pursuing stroke center certification, want to expand your neurodiagnostic capabilities, or need teleneurohospitalist support to fill gaps in coverage, our customizable solutions can provide help.
Expand access to benefit patients
Vituity provides 24/7 access to a dedicated panel of board-certified neurologists and the latest teleneurology innovations, and our integrated solutions work within your EHR, infrastructure, and culture.
Coordinate care to improve patient experience
With our unique ownership model, neurologists are part of an integrated team of acute care experts that collaborate closely with the emergency department, inpatient unit, and ICU to treat your patients’ most complex neurological conditions.