Patient satisfaction, which now accounts for a significant percentage of Medicare fee-for-performance payments, is closely tied to patients' interactions with their care team. Unfortunately, a study out of Vanderbilt University showed that 82 to 90 percent of recently discharged inpatients couldn't actually name their provider.
The situation is even more difficult in the busy, chaotic emergency department (ED). ED patients are often stressed, anxious, and in pain. Under these conditions, it can be tough for them to retain information — even when it's clearly presented. For example, a patient who's in pain may hear that tests X, Y, and Z were ordered, but only remember Y and Z. So when X happens, they feel even more confused and overwhelmed.
Patients also come to the ED unsure what to expect. Some believe that when tests are ordered, the results will be back in minutes. (This is the emergency room, after all!) Others worry that results will take hours — or even days like they do in the outpatient setting.
Providers can help to relieve patients' anxiety and confusion with good communication. But of course, we can't be with the patient every minute.
So a group us got to thinking: wouldn't it be great if there were a tool that could help us communicate with patients and families — even if we're not in the room?
And then we realized there could be.
Tools for Better Communication
Over the past several years, Vituity has supported the development and testing of patient-provider communication tools at practice locations across the organization. The project was coordinated by Alice Kim, DO, ED medical director at San Joaquin General Hospital in French Camp, Calif.
The team looked specifically at two tools: communication boards and care cards. Both tools provide a constant reference point to help patients, families and team members know what's going on with patient care. And by empowering and educating patients, they help to make care more patient-centered.
Each location designed its own tools, but they shared a few crucial elements:
- Provider name
- Turnaround times of diagnostic studies (labs, x-ray, CT, admission times)
- Care plan and disposition
Let's take a closer look at each of these tools.
Communication White Boards
A communication board is dry-erase board with charts and graphics printed on its surface. The boards are located in each patient room and filled out by the team during each patient encounter.

A key advantage of the board is that it's always visible to the team, patient, and family. Everyone can see that plan of care at a glance. Medical Directors and nurse leaders can audit the board's use simply by glancing into the room.
On the downside, communication boards can be quite difficult to alter once they're created. Also, they must also be cleaned after every encounter to avoid confusion. Providers using the boards need to carry whiteboard markers next to their name badge and stethoscope, as it is difficult to keep the marker consistently present in the room.
Patient Care Cards
A care card is a paper version of the communication board that's filled out and handed to each patient. A nice thing about care cards is they can be personalized with the provider's photo and bio. Unlike the boards, they can be used in any part of the department, including the waiting room and hallway.
Some examples from our Vituity EDs:
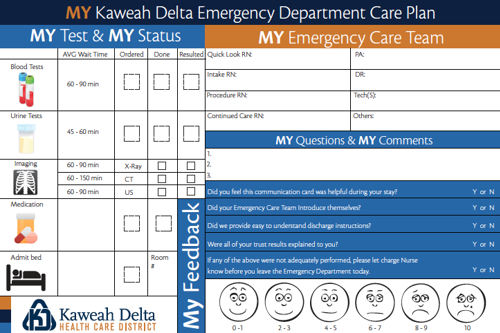
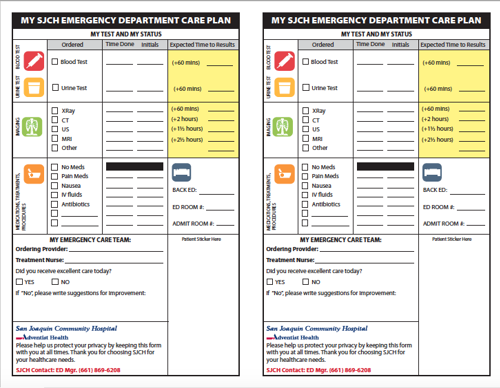
Care cards are much easier to update than communication boards. Want to add a new test to the list or change a time parameter? Simply edit the Word file and send it off to the printer for a new batch.
Of course, the printing of care cards is a recurring expense. Another disadvantage is that it's easy for hurried providers to "forget" or "run out" of care cards. Use of the cards is difficult to audit, because the patient may slip the card into a purse or pocket. And finally, the small print on the cards can be difficult for some patients to read.
Benefits of Communication Tools
Communication tools have two major benefits for patients and their care teams.
First, the tools help to manage patient expectations. When expectations are reasonable (for example, blood work results will be back in one hour), it's easier for our teams to meet and exceed those expectations — particularly when we use the "Disney" approach of listing wait times that are a bit longer than what we usually deliver. And this of course boosts patient satisfaction scores.
We've also seen firsthand how tools empower patients to participate in their own care. For example, let's say you've ordered urinalysis, but no one has given the patient a sample cup. The patient sees the order on the board, and of course, they want to go home as soon as possible. So they speak up and ask for the cup, and a potential delay is avoided.
The committee is still gathering outcome data on the program, but preliminary results show that the tools have a positive effect on throughput. For example, turnaround time to discharge (TAT-D) at Swedish Medical Center — Edmonds Campus decreased 5 minutes in the month after the rollout of the communication boards. Clearly communicating at the beginning of the visit that we needed urine meant less time waiting for a specimen, and communicating to the family that grandma would be going home helped ensure her ride would be waiting when she was ready for discharge.
Lessons Learned
By far our biggest challenge in implementing the communication tools has been getting team members to use them consistently. Here are some of the lessons we've learned.
Get buy-in prior to implementation. Success of the program requires collaboration among administration, providers, nursing, ancillary staff, and technicians. One way to create this buy-in is to involve the stakeholders in the tool's design. Care cards and communication boards should be designed by the providers and nurses who will actually be using them. Often this exercise sparks helpful discussions on reasonable timeframes, workflows and priorities for care. And the more people who get involved in the design, the more champions you will have when the tool is rolled out.
Audit use. Physician and nursing leaders need to monitor use of the tools closely, especially in the first few months (not just weeks) of implementation. Is the card being given to every patient? Is the board being erased after every encounter? Are team members carrying whiteboard markers in case the one in the room "disappears?"
Persevere. Remember, culture change takes months to become habit. The implementation period can be tedious, but the payoffs — smoother workflow, satisfied patients and families — are worth the effort.
To learn more about how Vituity can boost your ED's quality metrics, visit our emergency medicine page.
Originally published June 18, 2014. Updated September 11, 2018.


























