As emergency department (ED) volumes rise across the country, departments are looking for new ways to improve operational efficiency and reduce wait times for patients. Mercy San Juan Medical Center in Carmichael, Calif., decided to tackle the problem by boosting its ability to care for lower acuity patients in the ED's front end. The following is adapted from a poster presented at Vituity's annual conference.
Why Focus on Fast Track?
A few years ago, Vituity launched an initiative to bring turnaround time to discharge (TAT-D) under 120 minutes for all of its EDs. In the never-ending pursuit of throughput perfection, our team at Mercy San Juan Medical Center elected to focus on decreasing our Fast Track turnaround time.
Fast Track is a process that treats low-acuity patients (ESI levels 4 and 5) in the ED's front end. While this was already happening at Mercy San Juan, our team lacked a formal process for identifying these patients and moving them through the department. Nor did we have a dedicated Fast Track treatment area. Before the new initiative, low-acuity patients were spending an average of 139 minutes in the department — well above our parent system's benchmark of 100 minutes for this population.
We hoped that building an efficient Fast Track process would satisfy patients as well as improve our ED's overall turnaround time. By concentrating our efforts, we were able to design and assemble a new treatment process specifically for low-acuity patients that boosted efficiency and significantly reduced wait times.
Multidisciplinary Approach
At the Mercy San Juan ED, process improvement is led by the Team Care Committee, a vibrant group of physicians, physician assistants, nurse practitioners, nurses, scribes, technicians, registrars, and lab and radiology staff. The committee works to foster teamwork and find collaborative solutions to the department's challenges.
Over a three-month period, the Team Care Committee's five-member Fast Track Task Force successfully designed and launched the new Fast Track model. The task force took a true multidisciplinary approach to the redesign, meeting with and reporting to members of the committee.
Passion Transforms Process
The Team Care Committee broke down the Fast Track process into three major areas of concentration: patient selection, patient treatment, and discharge process.
By working together and concentrating their efforts on each of these three areas, the Fast Track Task Force was able to bring clarity to an otherwise complex challenge.
Task Force TAT-D Goal
Dignity Health (our parent system) had established a mean TAT-D goal of 100 minutes for ESI level 4/5 patients. The task force, with the support of the Team Care Committee, established a personal goal of 90 minutes, feeling that this was achievable in the long run and would benefit patients even more.
The Tools of Change
Patient Selection
Early on in the redesign, the Team Care Committee realized the importance of getting the right patient to the right treatment area, and that this concept was as important in Fast Track as it was in critical care.
With that in mind, the Task Force set out to develop specific Fast Track criteria that would be used to identify patients appropriate for Fast Track treatment and disposition.
A comment system was also developed for the lobby triage team to enter into the comment section of our EHR to help prepare the Fast Track Team for the specific needs each patient would require.
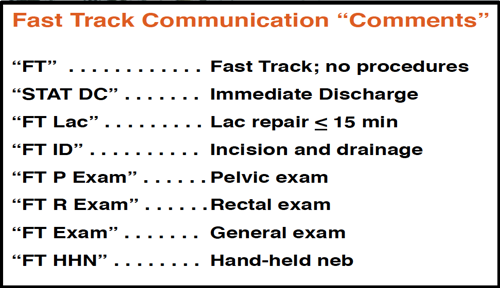
Patient Treatment
Once identified, Fast Track patients were taken to one of three Fast Track rooms for treatment. These rooms were specifically reorganized using lean concepts with two things in mind: speed and efficiency. The efforts in these rooms focused on three initiatives:
- Room reorganization: Each of the three rooms was reorganized utilizing lean concepts and 5S models to maximize efficiency. Although each room was equipped to "specialize" in specific treatments, all three rooms were organized with some redundancy to allow for flexibility.
- Dedicated staffing: Finding staff that were passionate about improving Fast Track and consistently wanted to work in that area provided tremendous "bang for our buck." Fast Track performed beyond expectations more often than not on the days these handpicked champions worked there.
- Team Assessment and Discharge: Assessing and discharging patients as a team had a tremendous positive impact on Fast Track throughput.
Discharge Process
The actual act of discharging the patient turned out to be just as important as Patient Selection and Patient Treatment in terms of throughput efficiency.
Designing an expedited discharge process (with input from the registration staff) helped minimize delays and got patients on their way quickly.
Under the new process, nurses discharged patients from any room or hallway chair after checking in with the provider to finalize prescriptions, work notes and other instructions. When possible,
Team Discharge (simultaneous discharge by both the provider and nurse) was used to improve efficiency.
There ended up being a key process change: if any patient who was ready for discharge still required full registration, then they took priority with the registration staff. After signing all the discharge paperwork, patients were escorted directly to any open registration window to complete the process. All discharge paperwork, including any prescriptions, was held by the lobby nurse to ensure patients completed registration.
Results
Despite large increases in ED patient volume during implementation, the project yielded exciting results. During this period, Fast Track mean TAT-D for ESI level 4 and 5 patients dropped 20 minutes. These impressive results speak to the value of a well-designed, highly concentrated effort at caring for this specific ED patient population.
Update
Since this poster was presented, ED volumes at Mercy San Juan have continued to rise, and the department has added quite a few new nurses and providers. While these changes have created some challenges for Fast Track, we are confident that the wealth of lessons learned will allow us to adapt to what appears to be a "new normal." We are fortunate to have several strong champions in the department who continue to advocate for this important aspect of our care.
Originally published June 4, 2015. Updated May 4, 2018.
























